Home
Subscription
April 2024 issue
April 1, 2024 issue
March 2024 issue
February 2024 issue
January 2024 issue
BACK ISSUES
2023
2022
2021
2020
2019
2018
2017
2016
2015
2014
2013
2012
2011
2010
2009
2008
2007
2006
|
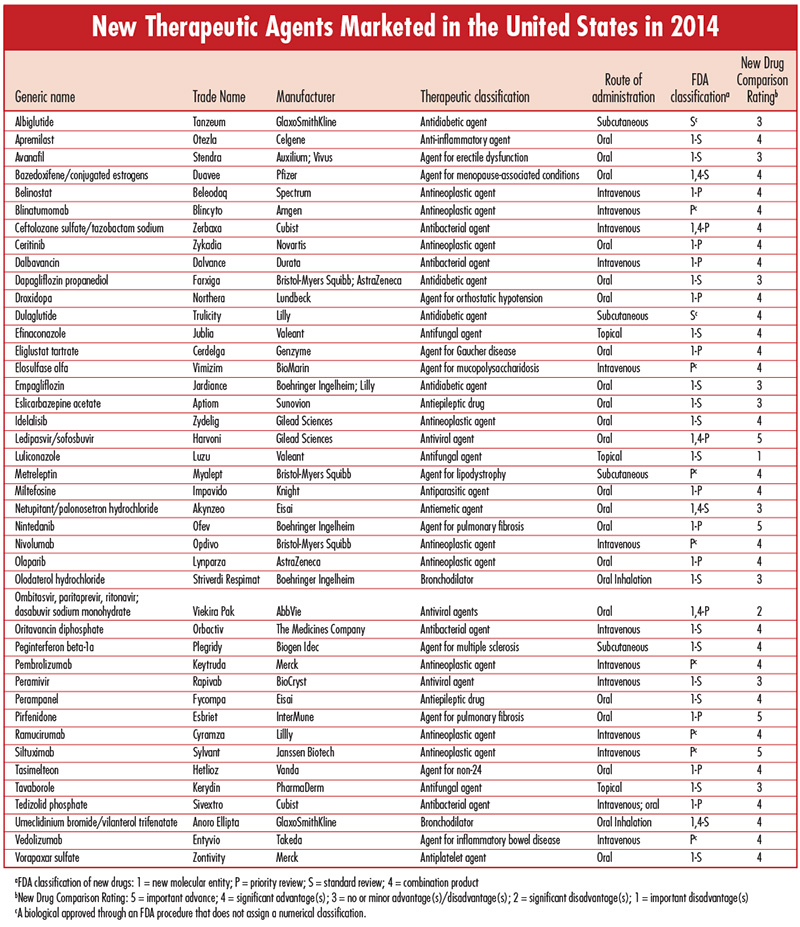
Each issue will include an editorial on a topic that is important for the profession of pharmacy, as well as a review of a new drug that includes a comparison of the new drug with previously marketed drugs that are most similar in activity, and a New Drug Comparison Rating (NDCR) for the new drug. Read on for this month's issue. August 2015 Issue [Download PDF format] In this issue: • Editorial • New Therapeutic Agents Marketed in the United States in 2014 |
|
EDITORIAL:
CVS Recommendations about the Cholesterol Guidelines are Not Credible When Its Pharmacists Do Not Have Enough Staff and Time to Practice OptimallyAlirocumab (Praluent) was approved in July and evolocumab (Repatha) in August as the first drugs in a new class of cholesterol-lowering agents known as the proprotein convertase subtilisin/kexin type 9 (PCSK9) inhibitors. They are more effective than previous agents in reducing low-density lipoprotein cholesterol (LDL-C; i.e., the "bad" cholesterol) concentrations, and represent important additions to the medications available for the treatment of hypercholesterolemia and reduction of its associated risks. Each of the new drugs has been specifically approved as an adjunct to diet and maximally tolerated statin therapy for the treatment of adults with heterozygous familial hypercholesterolemia or clinical atherosclerotic cardiovascular disease, who require additional lowering of LDL-C. Both drugs are administered subcutaneously and are expensive (approximately $15,000 a year for therapy that will continue for many years for numerous patients).Prior to 2013, the guidelines for the treatment of patients with hypercholesterolemia included specific target cholesterol concentrations. In 2013, the American College of Cardiology (ACC) and American Heart Association (AHA) released revised guidelines that do not identify specific cholesterol targets, but rather emphasize the consideration of multiple risk factors and appropriate (e.g., high-intensity) statin therapy. There have been differences of opinion regarding the revised guidelines even before the approval of the PCSK9 inhibitors. However, the approval of the new drugs has prompted CVS Health to recommend a return to guidelines that include target LDL-C concentrations (in a commentary that was published online on August 10 in the Journal of the American Medical Association). The CVS recommendationThe CVS commentary is authored by three physicians who are employed by CVS. Because CVS is primarily identified as a pharmacy company, it is noteworthy that none of the authors of the commentary is a pharmacist. Does CVS management feel that none of their pharmacists have the expertise and credibility regarding drug therapy management and clinical guidelines to participate as a coauthor of such a commentary? Or perhaps the pharmacists at CVS did not agree with their company's recommendation, and they did not want to be identified with it.The CVS commentary includes the following statements:
"The best approach will be to promote use of low-cost statin medications rather than PCSK9 inhibitors, but this approach will be complicated by recent changes in recommendations for treating hyperlipidemia."
I consider the last of the above statements to be highly insulting to practicing physicians and other prescribers. Even though most prescribers do not know the cost of medications, they recognize their responsibilities, and patients and society expect them "to simultaneously consider multiple competing priorities in clinical decision-making." This is not a new responsibility that they will be "forced" to accept if specific LDL-C target concentrations are not included in cholesterol management guidelines. "...the release of the ACC/AHA cholesterol management guidelines in 2013 fundamentally altered the way cholesterol-lowering medications are prescribed and inadvertently limited the ability of payers to employ typical utilization management tools." "...the recent ACC/AHA guidelines abandoned the longstanding principle that clinicians should treat patients to a specific LDL-C target." "...the guidelines do not recommend titration of therapy based on LDL-C control. Will clinicians interpret the guidelines to indicate that the highest-risk patients should be prescribed PCSK9 inhibitors? Perhaps most concerning from a social cost point of view, will relatively low-risk patients be considered for PCSK9 inhibitors?" "... a rational step-wise approach that again utilizes specific LDL-C target levels would help. In the absence of such an approach, clinicians will be forced to simultaneously consider multiple competing priorities in clinical decision-making: efficacy, safety, evidence quality, as well as responsible stewardship of limited health care budgets." Implications of the CVS recommendationThe CVS commentary identifies two valid concerns. First, the cost of the PCSK9 inhibitors and the large number of patients who will be candidates for their use over a period of many years will result in a huge cost that must be addressed. Second, the PCSK9 inhibitors will be prescribed inappropriately for some patients. However, for CVS, the second concern is part of the first because they anticipate that the new drugs will be prescribed inappropriately for some patients who could be effectively treated with less expensive conventional regimens, resulting in higher costs. The motivation for the CVS recommendation that target LDL-C concentrations be returned to the cholesterol guidelines is based solely on economics. If the cost of the PCSK9 inhibitors was similar to that of the statins, would CVS be urging a change in the guidelines? The answer is "No." Although the cost of the new drugs is a very important issue that must be effectively addressed, implementation of the CVS recommendation would result in what I consider to be even greater concerns.The CVS organization includes CVS Caremark, one of the largest pharmacy benefit managers (PBMs) in the country. The current policies of CVS Caremark and other PBMs have already created barriers and a bureaucracy (e.g., prior authorization, high co-pays) that compromise the authority and treatment options for prescribers and are a disservice to patients. The consequence of the CVS recommendation will be to enable its PBM to treat a "number" (i.e., the LDL-C) rather than a patient. If a target LDL-C concentration is included in respected guidelines, it will be much easier for a PBM to deny, delay, or otherwise restrict coverage of a PCSK9 inhibitor based on criteria that are constructed around the LDL-C. The current guidelines include an emphasis on the consideration of multiple risk factors, something that employees of a PBM are not in a position to do. By establishing financial and other barriers with respect to patients being provided with certain medications, the PBMs have significantly intruded into the authority and responsibilities of the health professionals who personally see, evaluate, and care for patients. It is the height of arrogance for CVS and other PBMs to contend that they are in a better position to make therapeutic management decisions for patients than the physicians and other health professionals who are directly and personally involved in their care. Alirocumab was approved and available for use before evolocumab. However, to be in a better position to negotiate prices, CVS made a decision to wait until evolocumab was approved before adding either or both agents to its list of covered medications. There are patients who would benefit from having treatment with a PCSK9 inhibitor initiated at the earliest possible time. However, CVS has denied the timely availability of alirocumab for such patients, and again demonstrates that it gives priority to the cost of the drug rather than to the best interests of patients. A better ideaCVS employs thousands of pharmacists. Why could these pharmacists not play an active role in communicating with prescribers and patients for whom cholesterol-lowering medications are indicated. This would contribute to the provision of optimal therapy for patients, collaborative working relationships with prescribers, AND more cost-effective drug therapy. Oh, but wait! Most CVS pharmacists do not have time to participate in such communication and services. They do not have enough staff and time to take care of even the most basic responsibilities in dispensing prescriptions, and are intimidated by the metrics that appear to be based on the strategy of turning out more prescriptions faster.CVS has the expertise and potential within its own company (its pharmacists!) to facilitate the appropriate use of the PCSK9 inhibitors, and to discourage their use in patients for whom conventional therapy is effective and safe. Such an approach would benefit patients, provide professional fulfillment for its pharmacists, and increase the respect and appreciation of patients for the services the pharmacists provide. CVS has a great opportunity! However, it would require a commitment from CVS management to provide more staff and time for its pharmacists to engage in this responsibility. The CVS recommendation to identify a target LDL-C concentration is self-serving and based solely on drug cost considerations. If CVS ignores/rejects the opportunity to involve its own pharmacists in the provision of optimal and cost-effective use of cholesterol-lowering medications, its recommendation that others take an action for which the sole motivation is the cost of the medication is not credible. Daniel A. Hussar
|
|
| |